Millions of Americans miss out on critical hours of shuteye every day, and this epidemic of insufficient sleep holds critical implications for all of us.
How well did you sleep in the past week? If you’re like many Americans, busy schedules, sleep troubles, families, stress and other things may have kept you from getting enough rest at least one or two days, possibly even more.
While awareness of healthier sleep habits and the benefits of rest has been growing due to increased research and public health campaigns, trends still show many people of all ages simply aren’t sleeping enough.
At first thought, sleepy people may not seem like such a big deal, but the reality is a sleep-deprived society is less healthy and more dangerous. Read on to learn about the implications of America’s lack of sleep, who is most affected, and how to get better rest.
Insufficient Sleep is Major Problem; Here’s Why
It’s estimated that between 30% Verified Source Centers for Disease Control and Prevention (CDC) The United States’ health protection agency that defends against dangers to health and safety. View source and 40% of Americans regularly miss out on adequate rest, described as at least seven hours each night. While certain groups are more likely to be sleep-deprived, it’s something that can affect anyone.
Between 30% and 40% of Americans regularly miss out on adequate rest, described as at least seven hours each night.
Even if you sleep well most of the time, when family members, coworkers and fellow drivers are sleep deprived, insufficient rest can even have indirect effects. Let’s take a look at what it means when people aren’t getting enough rest:
- They have higher risks of disease. Regularly getting getting less than seven hours Verified Source National Library of Medicine (NIH) World’s largest medical library, making biomedical data and information more accessible. View source of sleep increases your risk of obesity, heart disease, diabetes, high blood pressure, and other chronic illnesses.
- They may have impaired cognition. Sleep deprivation affects the mind in many ways, with research improving impairments Verified Source National Library of Medicine (NIH) World’s largest medical library, making biomedical data and information more accessible. View source to short and long memory, learning, decision making, creativity, attention, reaction time and motivation.
- They’re more dangerous on the road. Driving drowsy produces impairment after 18 hours of wakefulness, and tired drivers are conservatively linked with over 100,000 accidents, 71,000 injuries and 1,550 deaths each year.
- They make more errors at work. Due to cognitive impairments, people are more likely to make errors on the job when fatigued. Research on pilots, nurses and doctors, police officers, drivers Verified Source National Library of Medicine (NIH) World’s largest medical library, making biomedical data and information more accessible. View source and others all show increased impairments following sleep loss, and one study estimates that insomnia results in 274,000 workplace accidents per year costing $31 billion dollars.
- They may have worse mental health. Sleep deprivation is associated with increased depression Verified Source National Sleep Foundation Nonprofit focused on educating about sleep health. View source risk, increased emotional reactivity, Verified Source National Library of Medicine (NIH) World’s largest medical library, making biomedical data and information more accessible. View source more negativity among couples, and higher risks of mental health issues. Verified Source Harvard Health Blog run by Harvard Medical School offering in-depth guides to better health and articles on medical breakthroughs. View source
- Their children are more likely to be sleep deprived and overweight. Children of parents who don’t get enough sleep are more likely to miss sleep themselves, and they are also more likely to be obese. Sleep deprived kids tend to perform worse at school as well. Verified Source National Library of Medicine (NIH) World’s largest medical library, making biomedical data and information more accessible. View source
The Face of Sleep Deprivation in the U.S.
The consequences of sleep deprivation are serious issues from a public health and safety standpoint, and studying these trends in different communities can shed insight into who isn’t getting enough sleep, why, and how to improve. Here’s a look at the current research on sleep trends and what they might mean for you.
Differences by State and Region
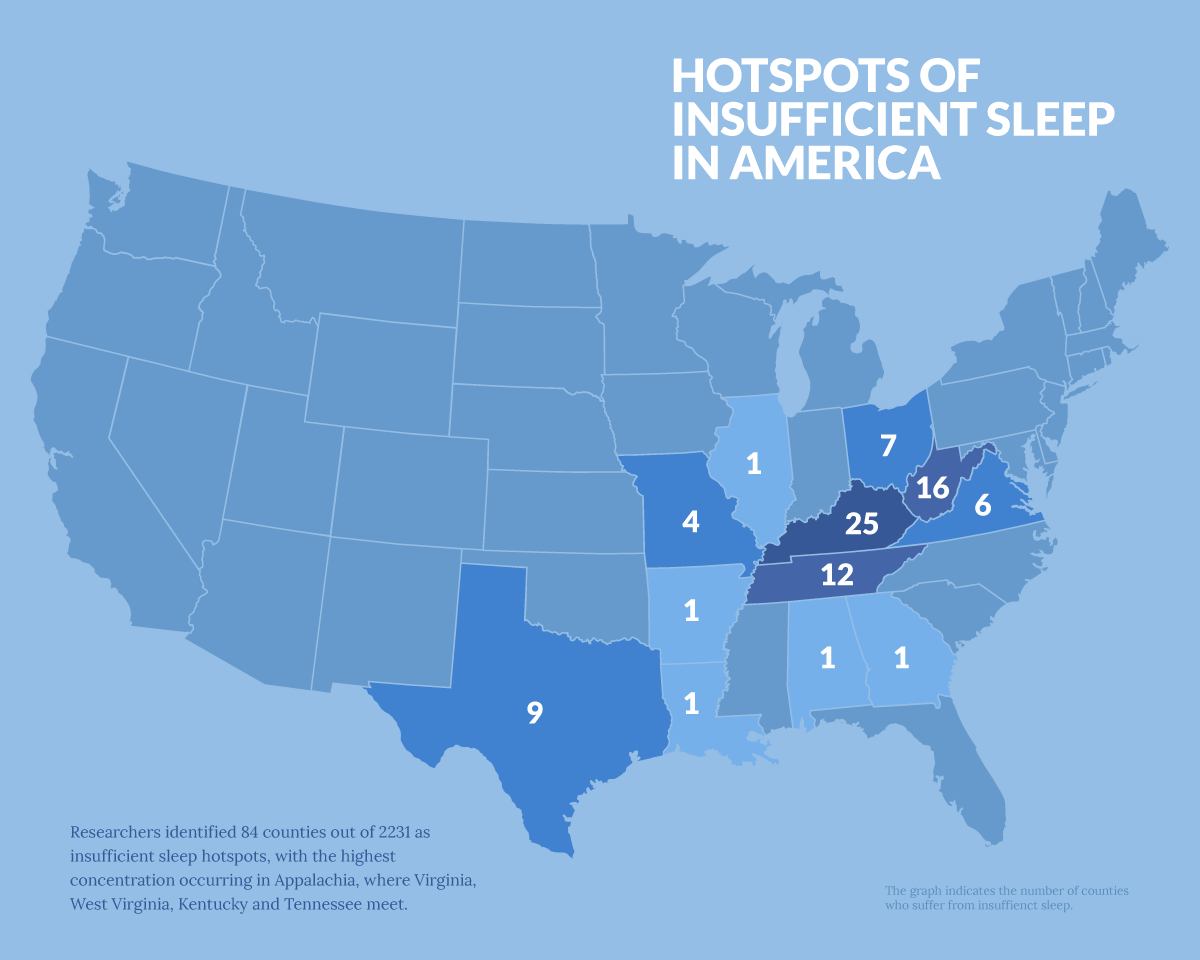
A recently published study in the Sleep Health journal looked at county-level trends to identify “hotspots” of insufficient sleep in America. Researchers identified 84 counties out of 2231 as insufficient sleep hotspots, with the highest concentration occurring in Appalachia, where Virginia, West Virginia, Kentucky and Tennessee meet. Overall, hotspots were found in:
- 25 counties in Kentucky
- 16 counties in West Virginia
- 12 counties in Tennessee
- 9 counties in Texas
- 7 counties in Ohio
- 6 counties in Virginia
- 4 counties in Missouri
- 1 county each in Alabama, Arkansas, Georgia, Illinois and Louisiana
On the other hand, “coldspots”, where people had very low levels of insufficient sleep included 12 counties in Virginia; 7 in Texas; 6 in Wisconsin, Illinois and Iowa; 2 in Georgia and Michigan, and 1 in Alabama, Minnesota and North Carolina.
No clear demographic pattern was identified for coldspot counties, but in the hotspots, people were more likely to be white, younger, of low socioeconomic status, and in poorer health.
In the high-concentration Appalachia area, study authors report that populations are at also at higher risk for obesity, heart disease, diabetes and other illnesses than elsewhere in the nation, also commonly identified as risk factors for poor sleep and effects of insufficient sleep.
A 2008 analysis Verified Source Centers for Disease Control and Prevention (CDC) The United States’ health protection agency that defends against dangers to health and safety. View source by the Centers for Disease Control at the state level found that West Virginia, Tennessee, Kentucky, Oklahoma, Florida, Missouri, Alabama, Louisiana, and North Carolina had the highest rates of sleep deprivation, and a 2012 study Verified Source National Library of Medicine (NIH) World’s largest medical library, making biomedical data and information more accessible. View source also identified the highest rates in West Virginia, Alabama, Mississippi, Missouri and Oklahoma.
All three of the studies mentioned here show the more sleep deprivation in the Appalachian and Southeast regions of the U.S., which researchers speculate may be influenced by a general lack of education, employment, lack of access to care and infrastructure.
Effects of Age and Lifespan Trends
The 2008 CDC report identified that people under age 45, particularly in the 25 to 34 age group, were more likely to report sleep deprivation, while people over 45 were most likely to report no days of insufficient sleep in the month prior to the study.
In a Gallup poll from 2013, nearly half of people between ages 18 and 49 reported getting less than six hours of sleep, and people in this age range were also most likely to report feeling sleep deprived. By comparison, just one-third of people over age 65 reported getting less than six hours of rest on average.

Younger people tend to lose sleep due to lifestyle and social factors, with having young children being cited by Gallup as a key issue. Other factors Verified Source American Academy of Pediatrics (AAP) Professional society for pediatricians that aims to improve children’s health everywhere. View source that may play a role are a shift towards eveningness in adolescence, higher prevalence of electronics use before bed, schedules, caffeine consumption, and poor sleep hygiene. Verified Source National Library of Medicine (NIH) World’s largest medical library, making biomedical data and information more accessible. View source
Older individuals are more likely to experience insomnia, light sleep and tend to gradually shift towards morningness, according to one recent Swiss study. However, researchers found that older people complain less about their sleep and reported higher sleep quality and better daytime functioning than younger counterparts. With age, women took longer to fall asleep and men showed reduced deep sleep, but both genders actually showed improved sleep efficiency (time spent in bed compared to time spent sleeping).
Other research also suggests that how well people sleep between 30 and 60, predicts mental functioning decades later as they age. Rather than viewing it as time wasted, researchers say younger people might consider healthy sleep as an investment in their later mental and physical health.
The Impact of Gender on Sleep
Although sleep is a universal function, it appears that men and women also tend to differ on amounts of sleep and on the impact of insufficient sleep.
In the U.S., women are more likely to report insufficient sleep in the past month compared to men, based on the 2008 CDC report. Polls from the National Sleep Foundation Verified Source National Sleep Foundation Nonprofit focused on educating about sleep health. View source show women report more sleep difficulties than men, with higher rates of insomnia, restless leg syndrome and other disorders. Researchers suggest differences in sleep may relate to factors unique to women, including pregnancy, menopause, and changes to hormones over their lifespan.
A Cambridge University study showed a similar trend in Britain, where women averaged 11 minutes less sleep than men, despite spending 15 minutes longer in bed.
This sleep gap may be pretty significant, too, according to a study from Duke University. Their research suggests that women actually need more sleep than men, and that women are more susceptible to the side effects of insufficient rest. Sleep-deprived women have higher risks of heart disease, depression, stroke risk factors, more hostile and angry feelings, and increased inflammation markers, which can worsen pain.
Men aren’t in the clear though. One study found that under sleep deprivation, men tend to make riskier decisions while women tend to become more risk-averse. As an example, according to an American Automobile Association report, men are more likely to drive drowsy, to fall asleep while driving, and to be drowsy when involved in a crash. In particular, male drivers under age 25 exhibited the highest risk of drowsy driving crashes.
Occupational and Educational Trends
In the 2008 CDC study, people with a college degree or some college were less likely to report insufficient sleep compared to people with high school diploma or GED or less than high school education. People that were unemployed or couldn’t work were significantly more likely to report 30 days of insufficient sleep compared to employed or retired persons, students and homemakers, which researchers suggest may be due to higher stress, medical issues and other conditions.
Shift workers…are at higher risk for chronic sleep deprivation, insomnia, and sleep-related health problems.
The type of jobs people have can also play a role in their overall sleep quality. Shift workers Verified Source Harvard Health Blog run by Harvard Medical School offering in-depth guides to better health and articles on medical breakthroughs. View source in particular remain a key area of focus for sleep researchers, as they are at higher risk for chronic sleep deprivation, insomnia, and sleep-related health problems. Other research from the American Automobile Association Verified Source National Sleep Foundation Nonprofit focused on educating about sleep health. View source shows that night shift workers are also six times more likely to be in a sleep-related car crash.
A study analyzing data Verified Source National Library of Medicine (NIH) World’s largest medical library, making biomedical data and information more accessible. View source from different National Health Interview Surveys found people working in corporate management, transportation, warehousing, and manufacturing averaged the least amount of sleep, while people in agriculture, education, real estate and professional services averaged the most.Reversing the Insufficient Sleep Epidemic
Improving sleep at the personal level depends largely on education and attitude. Organizations like the CDC and National Sleep Foundation produce regular public awareness campaigns that aim to explain the benefits of getting healthy rest and discuss good “sleep hygiene” tips people can use in their daily lives. The key tenets of good sleep hygiene include:
- Following a healthy routine. Going to bed and waking around the same time every day, with little variation on weekends, is one of the best ways to support healthy circadian rhythms for people of any age. Consistency tells your body when to be alert and when to get drowsy. For people who work alternating shifts or experience jet lag that throws off routines, light cues Verified Source Harvard Health Blog run by Harvard Medical School offering in-depth guides to better health and articles on medical breakthroughs. View source may be important for moderating sleep-wake cycles (you generally want exposure to bright light while awake and darkness while sleeping).
- Optimizing sleep environment. A comfortable bedroom can play a significant role in rest. Although personal preference is important, research shows that darkness Verified Source National Sleep Foundation Nonprofit focused on educating about sleep health. View source is important for melatonin release and the cooler temperatures Verified Source National Sleep Foundation Nonprofit focused on educating about sleep health. View source also support better sleep. Upgrade to the best mattress, pillows, and bedding for your particular needs, too. Minimizing disturbances from sounds in and outside the home may also be important for sound sleep.
- Watching dietary sleep stealers. Many people know that stimulants like caffeine can delay sleep, but so too can spicy foods, fatty foods, and heavy meals too close to bed. On the other hand, studies link eating a balanced diet with plenty of water during the day, and simple carbohydrates Verified Source Oxford Academic Research journal published by Oxford University. View source in the evening with fewer sleep issues.
- Managing stress and pain. The 2015 Sleep in America poll showed that both stress and pain can significantly affect sleep, and the missing sleep exacerbates both stress and pain, creating a detrimental cycle. Developing healthy strategies to manage stress and minimize pain can help improve sleep, and better sleep can in turn support better health.
- Getting help when needed. Many people with sleep disorders don’t seek treatment; for example, it’s estimated that 80% to 90% of sleep apnea cases are undiagnosed. If you have extended difficulty getting to bed or find that you aren’t feeling well rested in the morning, don’t ignore the signs — even if you suspect you know the cause. There are many tools your healthcare provider can utilize to improve your sleep, from behavioral and lifestyle adjustments to medications.
- Making sleep a priority. People who make sleep a conscious priority also tend to get more rest, according the Sleep in America poll. Giving sleep a place in your routine and doing healthy things throughout the day, like getting moderate exercise, minimizing caffeine, and getting daily sunlight exposure, can all be helpful for sleeping easier at night.
Workplaces can also have a role in improving people’s sleep, by supporting healthy corporate cultures. Offices where a healthy work-life balance is respected, where napping isn’t frowned upon (during appropriate times and places of course), and with some flexibility in hours tend to have happier and healthier employees over time. And, well-rested employees perform better on the job and are more satisfied with their jobs, too.
Ultimately, we each hold responsibility for our own health, and the more you know about what constitutes good sleep habits, the better equipped you are to get good rest and identify potential problems early on.
Do you regularly get at least seven hours of sleep? What do you do, or what can you do to improve your family’s sleep habits?
About the author
Rosie Osmun, a Certified Sleep Science Coach, brings a wealth of knowledge and expertise to the health and wellness industry. With a degree in Political Science and Government from Arizona State University College of Liberal Arts and Sciences, Rosie's academic achievements provide a solid foundation for her work in sleep and wellness. With over 13 years of experience in the beauty, health, sleep, and wellness industries, Rosie has developed a comprehensive understanding of the science of sleep and its influence on overall health and wellbeing. Her commitment to enhancing sleep quality is reflected in her practical, evidence-based advice and tips. As a regular contributor to the Amerisleep blog, Rosie specializes in reducing back pain while sleeping, optimizing dinners for better sleep, and improving productivity in the mornings. Her articles showcase her fascination with the science of sleep and her dedication to researching and writing about beds. Rosie's contributions to a variety of publications, including Forbes, Bustle, and Healthline, as well as her regular contributions to the Amerisleep blog, underscore her authority in her field. These platforms, recognizing her expertise, rely on her to provide accurate and pertinent information to their readers. Additionally, Rosie's work has been featured in reputable publications like Byrdie, Lifehacker, Men's Journal, EatingWell, and Medical Daily, further solidifying her expertise in the field.
View all posts






